 |
|||||||||||||
|
|
|
Lung Ventilators Although artificial
ventilation of the lungs is less used in veterinary than medical
anesthesia, it is frequently useful and its use is occasionally
mandatory. The primary indication for artificial ventilation is
pulmonary hypoventilation, which may be caused by central depression,
muscle weakness or paralysis (for example, during the use of neuromuscular
blocking drugs), and thoracic trauma or surgery. It must be
noted that IPPV has profound effects on the distribution of pulmonary
ventilation and blood flow,
and systemic hemodynamics. For example, IPPV results in a significant
reduction in cardiac output, particularly in anesthetised horses,
but further discussion of these effects is beyond the scope of this
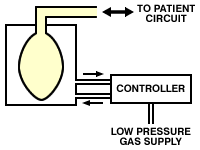
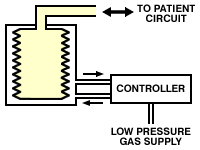
article. Types of Ventilator The classification of ventilators is somewhat complicated, and this is exacerbated by the fact that the same ventilator may function differently depending on how the controls are set. However, two of the most commonly used types of ventilator used in veterinary anesthesia are bag-squeezers and minute volume dividers. Ventilators designed for long-term ventilation in intensive care units are not usually suitable for use in anesthesia. Bag Squeezers As their name suggests, bag-squeezers replace the breathing bag, and usually also the pop-off valve, in the breathing circuit. Although some have been designed that compress the bag or bellows mechanically, using, for example, an eccentric cam or crank arrangement, most are of the bag-in-bottle type. Here, the breathing bag is enclosed in a rigid container and is squeezed by gas pressure applied to the inside of the container. The original bag has now usually been replaced by a concertina-type bellows.
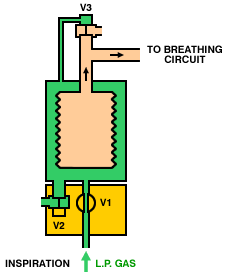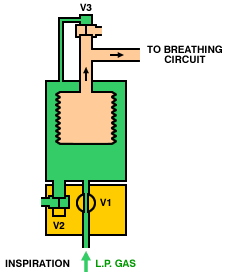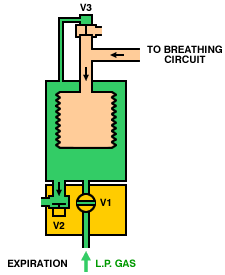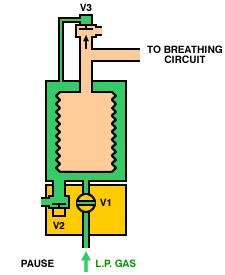
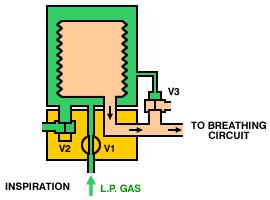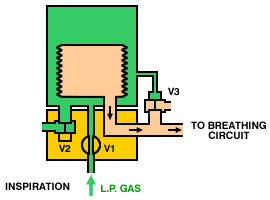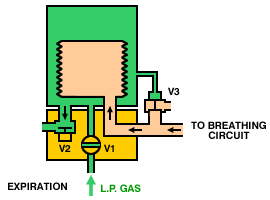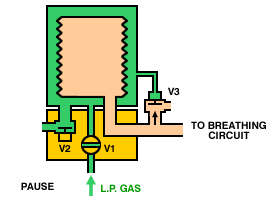
Operation of a typical bag-squeezer (below) is as follows. During inspiration, the inspiratory valve (V1) is opened, allowing gas from the low-pressure system to enter the container and squeeze the bellows. The expiratory valves (V2 and V3) are closed, so gas from the bellows is directed, via the breathing circuit, into the lungs. During expiration, the inspiratory valve (V1) closes, the expiratory valve (V2) opens and gas flows from the patient circuit into the bellows. Once the bellows is full, the pop-off valve (V3) opens and any excess gas is vented from the circuit.
Many older ventilators
of this type are of the descending bellows design, in which the
bellows hangs from the top of the assembly (as above). The problem
with this arrangement is that if the ventilator becomes disconnected
or the circuit develops a leak, the ventilator will continue to
cycle as normal (since, during inspiration, the bellows will be
squeezed and empty as usual and, during expiration, the bellows
will expand under its own weight and fill with gas from the atmosphere).
Bag squeezers
are used by substituting them for the breathing bag in circle absorber
systems (with the pop-off valve on the circle closed) and Mapleson
D systems (Modified Bain or T-Piece). They cannot be used in Mapleson
A systems (Magill or Lack) owing to the different position of the
pop-off valve in these circuits. Minute Volume Dividers In contrast
with bag-squeezers, which simply replace the breathing bag on an
existing circuit, minute volume dividers are self-contained circuits
which take the fresh gas flow rate, divide it up and deliver it
to the patient in individual breaths. It follows, again in contrast
with bag-squeezers, that the minute volume of ventilation is equal
to the fresh gas flow rate.
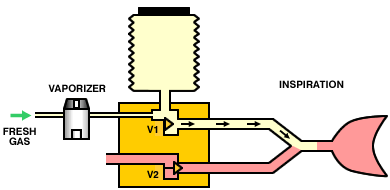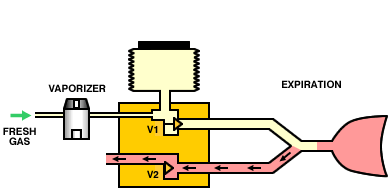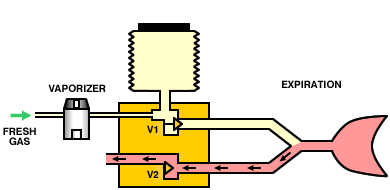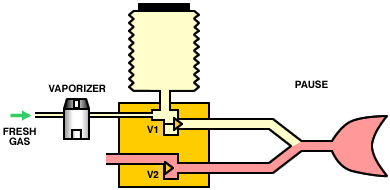
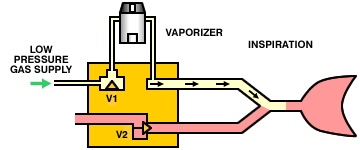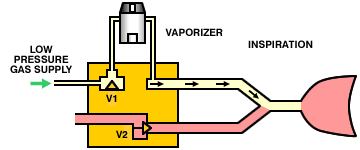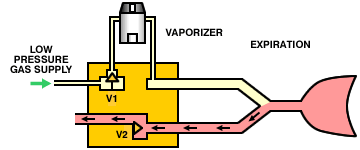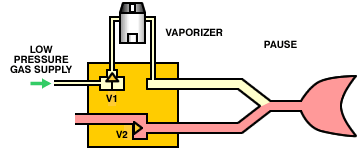
A variation on this theme is to replace the entire anesthesia machine with a microprocessor-controlled minute volume divider. The machine is connected directly to a low-pressure oxygen supply (there are no external flowmeters). During inspiration, the inspiratory valve (V1) opens, the expiratory valve (V2) closes, and gas flows through the vaporizer into the lungs. During expiration, the inspiratory valve closes, the expiratory valve opens and the patient exhales. The operation of the valves is controlled by a microprocessor which can calculate the required tidal volume and respiratory rate (and, therefore, minute volume) from the patient's body weight. By partially opening the inspiratory valve and opening the expiratory valve, the system can also operate as a Mapleson E circuit.
This provides a compact and convenient ventilator for small animal use. The very high flow through the vaporizer during inspiration (up to 60 l/min) may lead to inaccurate output and leaks. Controls Every ventilator needs a means of controlling tidal volume and respiratory rate. However, the method by which these are controlled varies widely between makes and models of ventilator. For example, tidal volume may be controlled:
Similarly, respiratory rate may be controlled or influenced:
Settings that may be adjusted on different ventilators may include:
In view of the large variety of controls on different ventilators, it is impossible in the space available to give specific instructions on the use of every specific make and model of ventilator: users should become familiar with the operation of the ventilators that they have in their facility. However, some general guidelines can be offered:
|
Comments on this
article should be addressed to Dr Guy
Watney
All pages © Anesthesia Service
and Equipment 1998-2003.